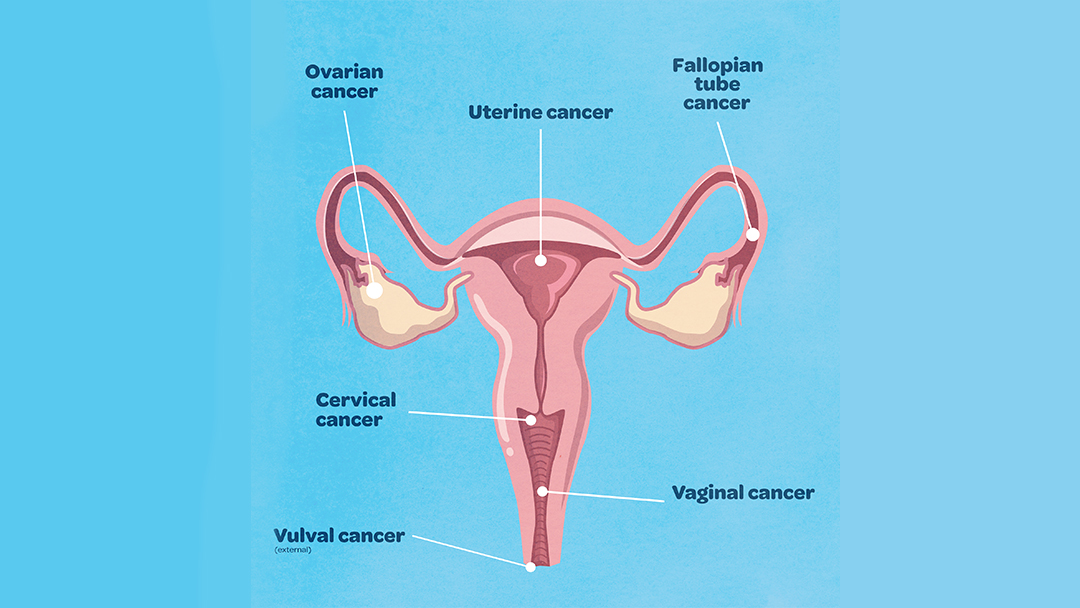
Uterine Cancer
- Happens in post-menopausal age
- Young women
- Good prognosis
Risk Factors
- Estrogen
- Progesterone
- Obesity
- 2x-50lb overweight - 3x incidence
- >50lb weight – 10x incidence
- Nulliparity - incidence increased 2x
- Late Menopause – incidence increased 2.5x
- Hypertension and Hypothyroidism are associated.
Symptoms
- Bleeding
- 15% of the patients with postmenopausal bleeding will have endometrial cancer.
- Intermenstrual bleeding/spotting.
- Other signs & symptoms
- Vaginal Discharge (80-90%)
- Pelvic Pain, Pressure.
What to do if someone has symptoms
- Please do not panic, majority of cases it's not cancer.
- Consult your doctor for routine checkups.
Tests
- Ultrasound of the abdomen
- Endometrial Biopsy – if anything suspicious.
- Hysteroscopy guided biopsy – dilation and curettage.
- CT Scan/ MRI as necessary.
If Diagnosed with uterine cancer, then
- Meet your one surgeon to plan next.
- Imaging to stage the disease.
- Surgery is the mainstay of treatment followed by adjuvant therapy based on staging.
- Surgery in cancer is different from what surgery is done in benign conditions.
- Surgery includes:-
- Removal of the uterus with ovaries.
- Removal of draining lymph nodes.
- Omental Biopsy
- Visual evaluation and if suspicious – excision of peritoneal lesions.
- In Stage 2 – a radical hysterectomy has to be done.
- Incomplete surgery increases the chances of recurrence.
- Patients with incomplete surgical staging may require
- Revision surgery
- Addition of chemotherapy/radiation.
What After surgery
- Adjuvant treatment based on the pathology report.
- Regular Follow-up:-
- First 2 years – Every month.
- Every 6 months until 5 years.
A patient with uterine cancer wants to have a child
- Only in selected patients with early disease.
- Grade 1 disease limited to endometrium on MRI
- Require proper counseling and frequent follow-up.
- In consultation with the oncology team
Summary
- Uterine cancer is curable if detected early.
- Surgery is the mainstay of treatment and differs from those done for non-cancer conditions.
- Complete treatment and regular follow-up have high chances of cure.